Caring for your Breasts
Breast Health
Videos
Your First Appointment
Diagnostic Tests
Breast Health
Table of Contents
The links below take you directly to the Breast Health information you are interested in. Or please scroll to keep reading.
Know what’s normal for you
It’s completely normal for your breasts to change throughout your life. Starting with puberty, using the contraceptive pill, through pregnancy and breast-feeding, and again in menopause.
The important thing is to know what is normal for you, by getting into the habit of regularly examining your breasts.
Breast Self Examination and Check-up
Ideally you should do your breast self examination about a week after the first day of your period. It’s a good idea to do this in front of a mirror so that you can see, as well as feel any changes.
How to do a breast self-exam:
Stand topless in front of a mirror with your arms at your sides.
- Look for puckering, dimpling, or changes in size, shape, colour or symmetry
- Look for cracked, itchy or dry looking skin on or around your nipples
- Do your nipples look different than usual? Are they turned in (inverted) or out?
- Look at your breasts with your hands pressed down on your hips and with your arms raised overhead and the palms of your hands pressed together.
- Lift your breasts to examine the underside and check whether the folds underneath are symmetrical.
The next step is to use your hands to check for any changes.
There are a couple of ways to use your hands to check for any changes. Decide what works best for you.
- Lie flat on your back: this makes your breast tissue spread out, making it thinner and easier to feel for any changes
- In the shower: if your skin is slippery, your fingers will glide more smoothly over your skin and make it easier for you to spot changes
- Ask your partner to do it: it is very often the case that breast changes are picked up first by the woman’s partner. You can help them by telling them what to look out for.
This is how I examine my patients’ breasts:
- Use the pads, not the tips of my fingers: I use my first three fingers as it means that I cover a larger area with each impression
- Adjust pressure levels: light pressure helps me feel the tissue closest to the skin, medium pressure to feel a little deeper, and firm pressure to feel the deeper tissue. I use all three levels before moving on to the next spot.
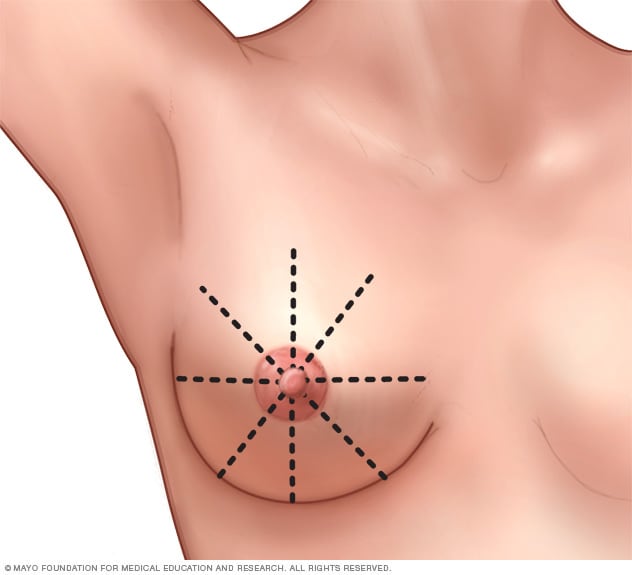
- Imagine a clock-face: it’s important that you are methodical to ensure that you are thorough. The way I do it is to imagine the face of a clock over your breast. I begin near your collarbone and examine that section, moving my fingers toward your nipple. Then I move my fingers to 1 o’clock and so on. Remember that there is breast tissue in your armpit, so I always check there too.
Book your Mammogram
From the age of 50 (or before if you have a concern) you should have a regular mammogram every 2 years. These are free, and you may see a mobile breast screening facility in your area. Mammograms are great for the early detection of disease. Unfortunately women with large or particularly dense breasts may find this procedure uncomfortable, but it is over quickly and your health is worth it!
Dense Breasts
If your breasts are particularly firm, there is a chance that a mammogram could miss cancerous tissue. If this is a concern for you, then get a referral to a breast surgeon, as we have other, more sensitive tests that would be more suitable and/or more comfortable for you.
Your breasts and puberty
Puberty can be a confusing time. There are so many changes happening in your body and your mind, so its useful that you know what to expect. Knowing your body is the best means of looking after it and keeping it safe and well. Knowledge is power, and if you are well informed, you will navigate the challenges of puberty more easily.
When will I get breasts?
Breasts often start to develop from the age of 9 to 11, give or take a year or two. The age when they start to grow or how fast they grow doesn’t mean that they will be big or small, the two things are not connected.
Your breasts are amazing organs. They have everything you need to one day feed a baby, if that’s going to be part of your story. When they start to grow, it means that you are beginning to transform from a girl into a young woman.
What should I look out for?
As your breasts start to develop, you’ll notice a small bump, called a breast bud, that appears under your nipple and areola (the darker area of skin around the nipple).
Fatty tissue and milk-producing glands will grow under your skin and will make your breasts bigger and rounder. Your areola will get bigger and darker and your nipples may stick out a bit more and become more sensitive.
Your friends’ breasts might not grow at the same time or be the same size as yours, but that’s completely normal. It’s really unhelpful to compare, because each of you is perfect in your own way.
What does normal look like?

Don’t expect your breasts to look like the those you see in adverts or magazines. As a breast surgeon, I have seen thousands of breasts, none of them looked like the airbrushed, enhanced images you might see.
What does it feel like to grow breasts?
As your breasts grow, they may tingle, ache or itch and your nipples may swell or become tender. This is all normal. Taking regular painkillers can help, as can a hot water bottle or cold pack.
But if you are experiencing pain, rather than tenderness, or discomfort do go and get checked by a doctor, especially if your breasts feel hot or look red. It is understandable that you might feel self-conscious about doing this, but please be reassured – this what we do – day-in, day-out. There is nothing to be embarrassed about.
When you get your period, different hormones will be affecting your breasts during your cycle. These may make the breasts feel tender, painful or sore a week or so just before your period starts. It’s worth marking these days on your calendar, as you may also experience feeling sad or irritable at this time.
What if I don’t like my breasts?
In this age of Instagram, there is pressure on young girls and women to look a certain way, that simply isn’t realistic or real in most cases. Few of us get to be ‘perfect’ whatever that is, and if I could wave a magic wand, I would let women and girls love their healthy bodies perfectly as they are.
The shape and size of your breasts is determined by your genes. They are sisters, not twins, so they are unlikely to be identical. It is completely normal for your nipples to point forwards, out to the side or downwards, or even in slightly different directions.
It’s also normal for some girls and women to have hair around their nipples. If this bothers you, either cut the hair close to the skin, or clean the area with antiseptic and use clean tweezers. You don’t want to risk getting an infection or an ingrown hair so please be careful!
There isn’t anything you can do (other than surgery) to change the shape or size of your breasts, though there are many people, trying to sell you something, that might tell you otherwise. I strongly urge you to ignore them!
Should I wear a bra?
Wearing a bra will help support your breasts and make you more comfortable, especially during sport. As your breasts will change quite rapidly, you may find it helpful to go to a department store and get properly measured and fitted periodically. An ill fitting bra will be uncomfortable for you.
You might hear that bras with under-wiring can cause breast cancer. This has been widely researched and proven to be incorrect information. Please ignore anyone who tells you different.
My breasts are lumpy. Should I be concerned?
Breasts are either smooth or lumpy – both are normal, and this may change throughout your cycle.
If you find a lump in your breast that you’re worried about, see your doctor. It’s highly unlikely that there’s anything wrong, but a visit to the doctor will put your mind at rest. Feel free to take a friend or relative along with you, if you’d feel more comfortable.
Very occasionally lumps are a sign of a benign (harmless) breast condition, such as fibroadenoma. Find out more
Will I get stretch marks?
If your breasts develop and grow quickly, you may get stretch marks. Red lines may appear on the skin of your breasts or even on your thighs, hips or belly. Almost all girls get them during puberty, and they can occur if you suddenly lose or gain weight. They are also very common in pregnancy. Boys and men very often get them too, if they grow, gain weight or muscle mass quickly. They are a fact of life and completely healthy and normal.
Over time these stretch marks usually fade and are barely visible, and there isn’t a great deal you can do about it, though keeping the skin well moisturised may help, and some people think Vitamin E can help the marks fade more quickly.
Why are my nipples ‘leaking’?
Small drops of liquid appearing on the skin of your nipple is completely normal. It might happen after exercise or squeezing your breast or nipple.
The liquid is normally clear, but can also be yellowish to greenish or a brown/red colour.
Unless there’s a large amount of discharge from the nipple, this is nothing to worry about – though you can visit your doctor or practice nurse if you are worried by any discharge.
Why are my breasts so huge?
A few girls will develop excessively large breasts, out of proportion to the rest of their bodies. This is known as breast hypertrophy. We don’t really know why this happens. Girls with excessively large breasts are often self-conscious about their appearance and may suffer from backache.
A well fitting bra will really help, but they can be hard to find. Luckily there are specialist shops and online stores that can help you get a good fit.
www.bravissimo.com
www.debras.com.au
Dieting and losing weight won’t help reduce the size of the breasts for girls with breast hypertrophy. Surgery is really the only option for you, and if you are concerned you should ask your GP to refer you to a breast surgeon.
Your breasts, pregnancy and breast feeding
Following the birth of your baby, your hormones will be changing rapidly. At first your breasts will produce a substance called colostrum. This is ‘liquid gold’ and will provide your baby with extremely valuable nutrients and antibodies. Around the third day or so after the birth the colostrum becomes diluted by additional fluid that makes it look much whiter. Around this time your breasts may start to leak milk.
Many women worry that breast feeding will hurt, or that they won’t be able to do it. For most women, this fear is unfounded, but for others, it can take a bit of getting used to. Your midwife should be able to help you.
When your baby sucks at the breast it triggers nerves that carry messages to the brain that milk is needed. Some women find milk leaks from the nipple when they hear their baby cry, or if their breasts are full and they feel emotional.
This can happen quite a lot in the first few days after you give birth. Putting disposable or washable breast pads in your bra can help you feel more comfortable and prepared.
Some women choose not to breastfeed because they have had too many challenges, or they simply don’t feel it is the right choice for them and their baby. There isn’t a right or wrong decision; you just need to feel you have made the best decision for you and your baby.
Women who have had breast surgery – due to breast cancer, breast reduction or breast implants, for example – may find that they are unable to breastfeed. However, some women are still able to breastfeed after surgery. You can ask your midwife, health visitor or breastfeeding counsellor for help.
Potential breast-feeding challenges
Here are some of the challenges you may experience when your milk comes in. Most of them are temporary in any case, and support from your care team can help you cope and resolve any issues you may face.

Sore and cracked nipples
This is often a sign that your baby is not attached to the breast correctly. If your baby only sucks the nipple, rather than the whole areola being in the mouth, the baby’s tongue or roof of the mouth rubs on your nipples and they quickly become sore and sometimes cracked.
The nipples won’t heal if the baby doesn’t attach to the breast properly, so if feeding is painful it’s important to get support from a midwife or breastfeeding counsellor as soon as possible.
It’s possible that your baby can’t latch on properly because they have a tongue-tie, meaning that they can get their tongue out far enough. This is easy to solve, with just a quick incision to the membrane under the baby’s tongue.
Rubbing a little breast milk into your nipples can help, and in the short term, wearing nipple shields can protect your nipples until they heal.
Engorgement
Breast engorgement can happen when milk comes in and your breasts are too full of milk. They may feel painful, hard, hot and throbbing. Engorgement will usually pass in a few days. Feeding your baby will help, although you may need help getting them latched on properly. It might also help to squeeze or pump some milk out of your breast to make it easier for your baby to feed.
You may also find the following helpful:
- Wear a well-fitting nursing bra that doesn’t restrict your breasts
- If your breasts are leaking, apply warm flannels just before expressing
- Apply cold packs to your breasts after feeding or expressing milk. This may help to reduce pain and swelling
- Take paracetamol at the recommended dose to ease the pain. This is safe to take while you are breastfeeding
Blocked milk ducts
Sometimes a milk duct becomes blocked while breastfeeding. This can also happen when you stop breastfeeding. You may experience a small, painful, hard lump or a bruised feeling.
Things that may help include:
- Feeding your baby more often
- Changing position when you’re feeding (this may help to drain the area more fully)
- Gently massaging the lump towards the nipple while your baby is feeding
- Applying warm flannels to the breast
- Ensuring your bra and clothes aren’t too tight so the milk can flow freely
Mastitis
If breast engorgement or blocked milk ducts don’t pass, it is possible for your breast to become inflamed or infected. Your breast may be red, hot and painful and you may get flu-like symptoms including headache, nausea and a raised temperature. If this happens, it is important that you see your doctor as soon as possible, as you may need a course of antibiotics.
It’s important to continue to breastfeed frequently, as this helps to clear the infection and is not harmful to the baby.
Breast abscess
If mastitis or an infection isn’t resolved, some women go on to develop an abscess (a collection of pus) in the breast. Breast abscesses are not common – if you think you have an abscess it is very important to see your GP. They may refer you to the breast clinic at your local hospital.
Abscesses can usually be treated with antibiotics and are often drained using a needle and syringe. An ultrasound scan may be used to guide the needle into the correct place. If the abscess is large, a small cut is made in it to allow the pus to drain away. An injection of local anaesthetic is usually given to numb the area first.
Occasionally, breast surgery is needed to remove the abscess. It’s usually a pretty straightforward procedure with minimal scarring, and perhaps a night in hospital.
Thrush
Some women get thrush on their nipples and areola during breastfeeding. It’s a yeast infection that can develop following cracking or damage to your nipple but may also happen suddenly, even when you’ve been breastfeeding for some time.
Your nipple may become itchy, painful and sensitive to touch. Some women find they have shooting pains deep in the breast that start after feeding and can last for a few hours.
Thrush can also be passed from mother to baby. Signs of thrush in your baby may include a creamy patch on the tongue or in the mouth which does not rub off, restlessness during feeding, pulling away from the breast and nappy rash (red rash or soreness that is slow to heal).
If you think you have these symptoms, talk to your GP or health visitor. Both you and your baby will need to have treatment at the same time.
What happens if I don’t breastfeed, or want to stop?
Breast milk is produced ‘to-order’, so if you don’t feed or express, your supply will soon dry up. You may find your breasts feel heavy, uncomfortable and sore for a few days. Wearing a supportive bra and taking pain relief may help.
Women continue to produce milk if breastfeeding continues. When you stop breastfeeding it may take some time for the milk production to stop completely.
If you stop breastfeeding too quickly, this can lead to engorgement. When you want to stop breastfeeding it’s best to gradually reduce the length and number of breastfeeds. You may like to start by dropping one feed a day. Your body produces milk on a supply-and-demand basis so this will naturally reduce the amount of milk you produce.
Milk may leak for several weeks after you stop breastfeeding if something triggers the ‘let down’ reflex (when hormones tell your breasts to produce milk). You may experience a tingling feeling in your breasts and nipples that can be quite strong, a feeling of sudden fullness, or you may notice that milk starts to leak from either or both breasts.
When you stop breastfeeding your breasts will most likely slowly reduce in size, although some women find that their breasts are larger than before pregnancy.
Your breasts after pregnancy
After pregnancy, whether you have breastfed or not, your breasts probably won’t look or feel the same as they used to. You may have gained or lost weight, and it’s not unusual to find your breasts have altered in size and shape compared with before pregnancy.
These changes are part of the normal changes your breasts go through at different stages in life. It’s important that you get to know how your breasts look and feel now so you can be aware of any new changes. You can find out more on our Checking your breasts page.
Benign Breast Conditions
Checking your Breasts for Lumps
Have a breast specialist check any changes in your breasts
Any changes in your breasts should be checked out by a breast specialist, if only to put your mind at rest. Your breast specialist will refer you for some tests such as a mammogram, ultra-sound, biopsy or an MRI
TYPES OF BENIGN BREAST CHANGES
Lumpy breast tissue
Known by doctors as localized nodularity, this is very common in younger women who may notice lumpiness at the outer edges of their breasts. This mostly happens as a result of hormonal changes e.g. puberty or stopping breast feeding.
If the lumpiness is the same on both sides and changes with the menstrual cycle), all you need do is get a check up from your specialist around every 2–3 months.
If the lumpiness is not symmetrical and/or there is thickening of the skin, then you should get checked out straight away, especially if you are over 30. Further investigation is probably called for.
Fibroadenomas
Fibroadenomas are harmless lumps of glandular and fibrous tissue. Breasts are made up of lobules (milk-producing glands) and ducts (tubes that carry milk to the nipple), and are surrounded by glandular, fibrous and fatty tissue. Typically, fibroadenoma develops from a lobule and later the glandular tissue and ducts grow over the lobule, forming a solid lump. Fibroadenomas in breasts may feel firm and rubbery and will have a smooth texture.
Fibroadenomas are not cancerous and do not increase the risk of breast cancer.
About one in six (15%) women have fibroadenoma at some time in their life. Fibroadenomas make up about 12% of all the non-cancerous breast lumps. They are most common in women aged 20 to 40. Fewer than 5% of women over 50 get them. Although, the exact cause of fibroadenomas is unknown, they are subject to hormonal influences.
Larger fibroadenomas (>3–4 cm diameter), with atypical features or those significantly increased in size should be biopsied regardless of patient age.
Most fibroadenomas can be left alone if they remain stable in size over time. Removal may be recommended if there is a significant increases in size, there is pain or if there is anxiety about the lump or if there are any features on imaging that raise concern.
Cysts
Cysts are fluid ‘bubbles’ in the breast tissue and common in women aged 35–50. They usually cease with menopause, but are common in women taking Hormone Replacement Therapy (HRT). Approximately 7% of women may feel a cyst at some point of their lives. Breast cyst are often not noticed and are usually found incidentaly on routine imaging. Cysts can also appear as lumps that are smooth, soft to firm, mobile, and sometimes tender. Cysts that are full can be firm to hard and tender on examination.
Cysts appear as well defined round densities on mammography. On ultrasound, cysts appear as well defined round or oval lumps. Sometimes it is recommended that some of the fluid is removed from the cyst so that the sample can be sent for analysis.
Cysts are harmless and do not increase your risk of cancer. But you should always get them checked out by a specialist just in case.
Fat Necrosis
Trauma or damage of breast tissue can lead to a lump formation known as fat necrosis (cell death). The damage to the fatty breast tissue can occur following breast surgery such as breast reduction and breast reconstruction, or radiotherapy to the breast. It can also result from direct injury or trauma to the breasts. Like other breast changes, you should always get it checked out, but fat necrosis is not harmful or a risk factor for disease.
Your First Appointment
Click here to learn more about your first appointment
Diagnostic Tools






For all appointments and enquiries, please call +61 2 8203 1359 or email info@drerickfuentes.com.au
Or contact us online using this form:
Request an Appointment Or Send a Message
Wise Medical
Level 1
11 Khartoum Road
Macquarie Park
NSW 2113
Strathfield Private Hospital
3 Everton Rd,
Strathfield NSW 2135
Hours: 9am - 5pm
Follow Us
© 2024 Dr Erick Fuentes. Breast and Endocrine Surgeon.